So far, more than 2,000 hospitals have been slapped with up to a 1 percent cut in Medicare reimbursement after they were deemed to have higher than average readmission rates for Medicare patients with pneumonia, congestive heart failure and acute myocardial infarction. A new report takes a look at some of the reasons behind avoidable readmissions and what can be done to improve it.
That penalty is set to rise from 1 percent to 2 percent this year as part of the Affordable Care Act and the list of conditions tracked will also increase. The goal is to reduce the $17 billion in healthcare costs the federal government says is caused by avoidable readmissions that take place within 30 days of patients being discharged from the hospital.
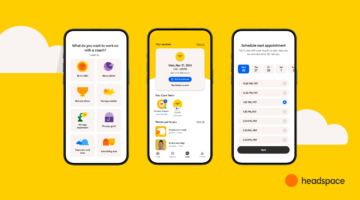
The Robert Wood Johnson Foundation in Princeton, New Jersey funded the two part report. One section by Dartmouth Atlas Projects crunches readmission rates from 2010-2011 across the country, region by region, and distinguishes between readmissions following surgery and readmissions for other medical reasons. There’s also an interactive map. A second section by Perry Undem Research and Communication interviews patients and providers to flesh out reasons for avoidable readmission and ideas towards improving it.
The most common reason for avoidable readmissions is that patients don’t understand hospital instructions and may not have a family member or another caregiver to ensure they do. There needs to be better care coordination once the patient is discharged, particularly with a primary care physician or other help An interactive map highlights the scope of the problem.
Among the other reasons cited by healthcare providers and patients for readmissions are:
Communication breakdown This frequently happens during the initial hospital stay at discharge process. Lack of clear instructions, incomplete information, questions not asked, and poor recall of the details. Hospitals are not ideal learning environments for ill, medicated patients. This can be especially true of medication. If medication is changed while patients are in the hospital and the
receiving physician is unaware, he or she may prescribe another medication that conflicts with that drug. Another problem is when patients get confused about a change in their medications are changed and providers don’t sufficiently explain the change.
Patients discharged too soon Financial pressure from administrators to discharge patients as soon as possible, especially under the current terms for reimbursement has been a factor. A number of patients felt they were discharged too soon and health care providers agreed this happens frequently. On the other hand, some patients said they wanted to leave as soon as possible.

A Deep-dive Into Specialty Pharma
A specialty drug is a class of prescription medications used to treat complex, chronic or rare medical conditions. Although this classification was originally intended to define the treatment of rare, also termed “orphan” diseases, affecting fewer than 200,000 people in the US, more recently, specialty drugs have emerged as the cornerstone of treatment for chronic and complex diseases such as cancer, autoimmune conditions, diabetes, hepatitis C, and HIV/AIDS.
Staff shortages This is a pretty big problem because with the number of newly insured people entering the system because of the Affordable Care Act, the problem of shortstaffed hospitals is expected to worsen.
Among the recommendations made in the report are:
Raise profile of primary care physicians Patients can lose touch with their primary care physicians when they’re hospitalized. Having a primary care physicians could better coordinate patient care and help patients with lingering questions or problems they are likely to face when they leave the hospital.
Start discharge process while patients are still hospitalized. In places where there was a greater tendency to use hospitals as the site of care, patients were more likely to be readmitted, regardless of illness levels.
Monitor physicians whose patients have high readmission rates This is one of the more controversial recommendations but given the reimbursement fines providers are facing, the authors think this may already be happening.
Outcomes improve for patients with a physician affiliated with the hospital This could help patients with follow up care and give them a logical contact when they initially get sick.
Referring patients to their own outpatient clinics If patients stay in the health care system, it allows for more effective care coordination.
Use patient navigators Navigators can help coordinate patient care from admission to helping plan for patients discharge by bringing in nutritionists and others who can give detailed information and help schedule follow-up care.
[Photo credit: Intentional motion blurred image of a business group from BigStock Photo]