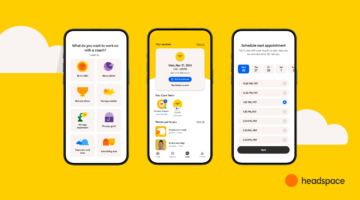
Arundhati Parmar, editor-in-chief, MedCity News interviews Cris Ross, CIO of Mayo Clinic at the HLTH conference.
Cris Ross is the chief information officer at Mayo Clinic, responsible for all information technology. By necessity, he is steeped in IT, but it wasn’t until he became a patient that he fully understood how his work affects providers and patients.
At HLTH’s Frontlines of Healthcare session, part of the Engage track created by MedCity News, Ross and MedCity News editor-in-chief Arundhati Parmar chatted last week about the lessons he learned from his experience as a cancer patient. Ross was diagnosed with stage 3 colorectal cancer and went through the customary trifecta: chemo, radiation and surgery.
“I had a routine exam and found out I had an advanced cancer,” Ross recalled. “I’m a CIO, so I’m used to bad news every day…The thing that came home for me the most was when I had a port placed for chemotherapy, and I realized: This is me and not somebody else.”
As Ross proceeded through his layers of treatment, he felt it was important to learn from his cancer, and he didn’t have to go far. Mayo had recently rolled out a new electronic health record and clinicians were still acclimating to the system. EHRs are complex, sometimes overwhelming, and they don’t always make it easier for providers. However, Ross was not prepared to see his clinicians stumbling so badly over his new system. It made him cringe.
“One of the big determinants of whether a clinician is happy with an electronic health record system …is whether they were well-trained for it, and have they set up their own customizations to use it the way they want…I don’t think we had done the best job,” he said.
Now that he is officially a survivor, he wants to make these systems more user-friendly. So Ross will focus on simplifying documentation – the tasks clinicians must perform to get paid or report on quality.
“You look at the length of a clinical note in the United States compare to the rest of the world,” Ross said. “It’s so much longer.”
Emerging technologies, such as automated transcription, could help mediate this issue. So-called “smart rooms” could pick up conversations between providers and patients, create notes based on best practice and even issue orders.
“It looks incredibly powerful, from our perspective, around what you can do to get the clinician to have a more or less natural interaction with the patient,” said Ross, “as opposed to dividing their attention between the patient and the computer.”
Ross feels most vendors have done a good job understanding the hospital experience, which he likens to a coral reef – a complex, interactive ecosystem. However, layering additional technologies on top of legacy systems is a challenging undertaking. New platforms may have a hard time supplanting the existing systems providers know well. Point solutions that do one thing, instead of addressing the larger picture, may also be problematic.
In addition to making internal systems more usable, Mayo recently announced a partnership with Google to move the clinic’s three petabytes of data to the cloud. The clinic uses the database to improve care. It also shares de-identified data with vendors to drive innovation, particularly in radiation therapy, genomics, image analysis and cardiology.
“We always wanted to get it to the cloud, but it took a while for the cloud vendors to develop enough healthcare-specific attributes that we felt it was time for us to move,” said Ross. “We have a roadmap of things that we want to do around discovery to bring machine learning, develop algorithms and speed the pace at which we can get those solutions from the lab to the bedside.”
Photo: HLTH