
EHRs have long been blamed for deep physician dissatisfaction. And given that Wisconsin-based Epic dominates the electronic medical records market, it has borne the brunt of physician ire. It’s not uncommon to hear wry humor like “Epic failure” from doctors tired of the administrative burden EHRs represent.
A simple Google search of the words “EHRs and physician burnout” yields numerous articles decrying how much electronic systems exhaust doctors. However, the chief executive of Epic contends there is not a high correlation between the two. In fact, in an interview with Healthcare IT News at the HIMSS conference in Orlando in February, Judy Faulkner challenged journalists to dig deeper into this and tell an accurate story.
“Here’s something I wish the press would do. And that is, the latest studies I’ve seen are showing that there’s not a high correlation between happiness with the EHR and happiness with their job and the problem of burnout. I think it would really help if the media understands that, and helps everyone else know it,” she declared.
Faulkner specifically referred to a KLAS study adding that it “concluded that there isn’t a whole lot of correlation” between doctor burnout and the EHR.
So we decided to heed Faulkner’s call.
The research Faulkner cites comes from KLAS’ Arch Collaborative, an EHR usability-focused initiative made up mostly of health systems as well as some vendors like Epic, Cerner and InterSystems. The data is not yet available online, but Faulkner and other Arch Collaborative members had early access to the information. KLAS sent MedCity a slide deck about burnout, physician fulfillment and the EHR. The deck contained the information Faulkner referenced, as well as other data. It is scheduled for publication this summer, but some of the information in the deck has been part of other KLAS reports. The study wasn’t commissioned by any specific organization.

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
The Arch Collaborative surveyed 6,849 physicians and advanced practice clinicians from member/participating organizations. According to the survey participants, EHRs are the second-leading contributor to physician burnout (47 percent) just behind “too much time spent on bureaucratic tasks” (54 percent).
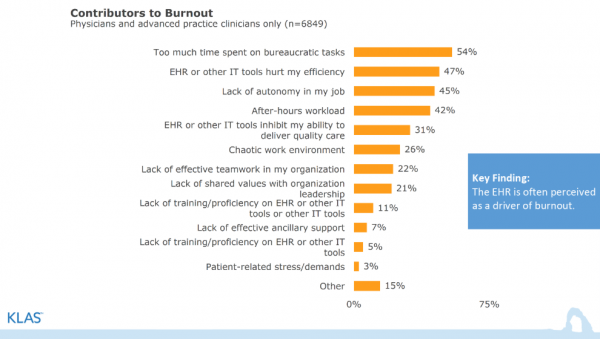
Source: KLAS – Arch Collaborative
Counterintuitively, however, the survey also found there wasn’t a huge connection between burnout and EHR net experience score.
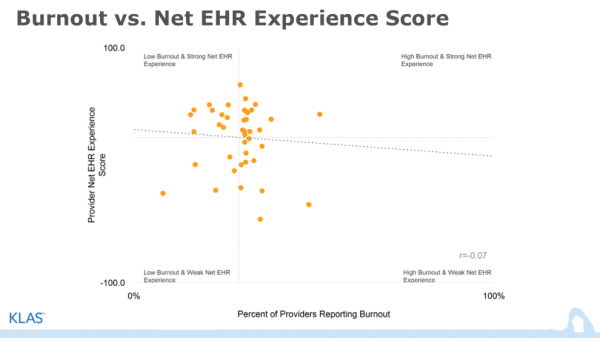
Source: KLAS – Arch Collaborative
“Clinicians report that EHRs are [a] top contributor to burnout, but when we look at organizational averages for burnout rates vs. organizational averages for EHR satisfaction, the correlation is low,” Taylor Davis, EVP of analysis and strategy at KLAS Enterprises, said in an email. He noted that while the EHR is frequently a problem for providers, fixing it won’t solve all burnout, as burnout is a multifaceted issue.
A separate study from the University of Notre Dame examined the tie between EHRs and physicians leaving the medical field. (The study was published in 2017 and revised in August 2018.) It found that basic EHRs have increased doctors’ tenure at hospitals, while advanced EHRs (or those that utilize computerized physician order entry or physician documentation) have caused doctors to move to other hospitals. It didn’t find any evidence of retirements as a result of EHR implementation. The researchers used information on physicians’ mobility from the Hospital Inpatient Dataset provided by the Florida Agency for Health Care Administration. HIMSS Analytics served as a resource for EHR implementation data. All information was from 2000 to 2010.
But other research has pointed to how electronic record systems take a toll on doctors.
Research published in Mayo Clinic Proceedings in 2016 concluded that “physicians’ satisfaction with their EHRs and CPOE [computerized physician order entry] was generally low. Physicians who used EHRs and CPOE were less satisfied with the amount of time spent on clerical tasks and were at higher risk for professional burnout.”
As part of a study published in 2018 in the Journal of the American Medical Informatics Association, researchers polled 1,792 practicing physicians in Rhode Island in 2017. Ninety-one percent of the respondents were EHR users. Of those individuals, 70 percent reported feeling health IT-related stress, which was defined as having at least one of the following: poor/marginal time for documentation, moderately high/excessive time spent on the EHR at home and agreement that using an EHR adds to daily frustration.
Additionally, 26 percent of the 1,792 respondents reported feelings of burnout. Notably, doctors who reported moderately high/excessive time spent on the EHR at home had 1.9 times the odds of burnout compared to those with minimal/no EMR use at home. Physicians who agreed that EHRs add to their daily frustration experienced 2.4 times the odds of burnout compared to those who disagreed.
Surveys and data are one thing. But what do one-on-one conversations with physicians reveal about the EHR and its relationship to burnout?
Dr. Louis Levitt, vice president of Bethesda, Maryland-based The Centers for Advanced Orthopaedics, appears to most closely echo Faulkner.
“I have not talked to many orthopaedic surgeons that have said, ‘Because of data demands and electronic record systems, … I’ve decided to retire early,'” Levitt said in a phone interview.
With more than 40 years of experience, Levitt is an orthopaedic trauma and joint replacement specialist and currently practices in the Washington, D.C. metro area. He added that it likely helps that orthopaedic surgeons have moved to using medical scribes or physician assistants, who can go into the EHR and help with documentation.
This is in stark contrast to what doctors in other specialties like primary care deal with. A commonly cited 2017 study from the University of Wisconsin and the American Medical Association found primary care physicians spent 5.9 hours out of their 11.4-hour workday in the EHR.
In Levitt’s experience, however, overwhelming practice demands are a lead contributor to doctor burnout. When it comes to EHRs, Levitt believes there are more pros than cons. Still, he acknowledged that it takes time to become facile at using Epic.
Dr. Jay Anders, CMO of computer software company Medicomp, has the opposite opinion on the correlation between doctor burnout and EMRs. “I think [the EHR] is contributing a lot,” he said in a phone interview. “It’s contributing more than people are going to give it credit for.”
While Anders, an internist, only does shifts from time to time, he spoke to his experience as a patient interacting with doctors who use EHRs. He said the three physicians he personally goes to are all on Epic, and they all hate it. Additionally, he recounted how the EHR has taken the personal interaction out of the visit. When Anders went to see his glaucoma specialist, for instance, the doctor entered the room and walked directly to the EHR without even saying hello to Anders.
To improve the EHR experience, Anders believes the federal government should create guidelines to which every state and every EMR vendor have to adhere. As for medical record vendors, Anders said they should get more physician input when designing and improving their tools. “I also think the big EMR vendors are slow to innovate or even listen to the physicians that are using their systems,” he said.
But it’s not just the EHR that’s responsible for burnout. Anders listed ever-changing regulations and the consolidation of medicine (i.e., practices being combined into large medical groups) as contributors to the problem.
A third physician, Dr. Valerie Jones, offered a unique and relevant perspective. She was a practicing OB/GYN up until two years ago when she decided to retire from a career in medicine at the age of 37. Jones wouldn’t necessarily say she was burned out, she explained in a phone interview. Rather, it was a combination of factors — including a personal health scare — that prompted her to leave.
Generally speaking, she does think the EHR contributes to physician burnout, mostly because of how much time it can add to the doctor’s plate.
“A lot of physicians go home with their computer now,” Jones said. “It can take time away from their families and take time away from their patients.”
The numerous requirements around what needs to be in the patient’s medical chart mean documentation can be time-consuming. Jones said that if someone came in with a cold or diabetes check, it can take four times as long to do it in the computer compared to writing it down.
The EHR is good for capturing costs, Jones noted, adding that they’re more geared toward capturing the billing information for insurance companies. But it “doesn’t really run smoothly from the physician’s standpoint,” she said. “For us, it should be about a safe way to document and tell a story about the patient.”
Circling back to Faulkner, it’s understandable why she would want to push back on the tendency to scapegoat the EHR/Epic for all physician woes and draw a straight line between EHR dissatisfaction and burnout. The reality is more complicated. However, it also appears that she is setting too low a bar when she says there isn’t a “high correlation” between EHRs and physician burnout. EHRs were meant to be liberating for doctors to help them better care for patients. Everyone would likely agree that they have fallen far short of that.
Photo: PeopleImages, Getty Images








