
Value-based payment models slashed hospital admissions and cut costs by $3.5 billion for people enrolled last year in Medicare Advantage plans offered by Humana, the Kentucky-based health insurer said in a report released Thursday.
The models also are prompting medical groups to invest in staff and technology, according to a survey cited in the report.

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
The report is the sixth annual look at the impact of value-based payments on the roughly 3 million members in Humana’s individual Medicare Advantage plans, as well as the thousands of providers who care for them.
Value-based payment models are seen as a way to lower healthcare spending and wring out unnecessary care, which is estimated to cost tens of billions of dollars per year. The models pay providers for improving health outcomes overall instead of on a fee-for-service basis, essentially asking providers to shoulder some of the risk that traditionally has been borne by insurers. But providers also can share in the savings if their patients stay healthy through preventive care, early intervention and other measures.
The challenge is engaging people in programs that encourage healthy behavior. Humana recently invested in a company, Accolade, that aims to spur greater engagement, at least through employer-based health plans.
The study looked only at people and providers in Humana’s Medicare Advantage plans. Under contracts with Humana, providers operate under a range of value-based payment models, with some accepting more risk than others but also gaining potentially more rewards.

Beyond Analytics: How Sellers Dorsey is Hard-Coding Value into Medicaid Policy [Video]
How to turn analytics into actual policy outcomes.
More than two-thirds, or 67%, of Humana’s individual Medicare Advantage members, were affiliated in 2018 with primary care physicians operating under value-based payment models. The figure was 66% in Humana’s 2017 report, though the insurer warned against making year-over-year comparisons due to annual fluctuations in its membership demographics.
If its members in value-based care models had been enrolled in Medicare’s traditional fee-for-service program, they would have incurred an additional $3.5 billion in costs, Humana said in its report, which was authored by a team of doctors. The savings stemmed from improved medication adherence and better management of patient treatment plans, among other factors.
Patients in value-based care also had a 27% lower rate of hospital admissions and visited emergency rooms 14.6% less often. And they were more likely to undergo annual wellness visits: 36.1% for members in value-based models versus 28% for those in non-value-based models.
The impacts extend to medical groups. As practices transition to value-based care, they are spending more on staff and technology, according to the survey cited in the report. It was conducted by the Medical Group Management Association in partnership with Humana.
According to the survey, 73.3% of respondents are adding staff and 65% are bulking up on technology

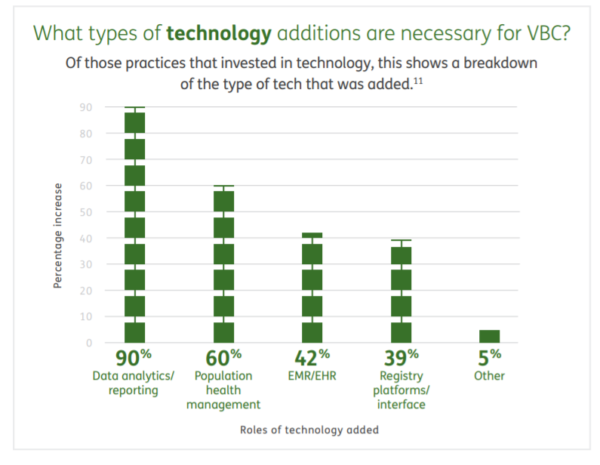
The most popular tools were data analytics/reporting, which were added by 90% of the practices that invested in tech, followed by population health management tools at 60%.
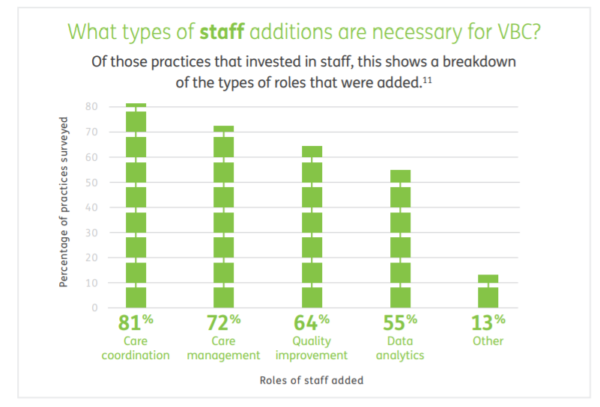
Staff is being added in areas such as care coordination (81%) and care management (72%).
Overall, medical groups in value-based models appear to be delivering better care, the Humana report found. For example, their patients were more likely to undergo preventive screenings. And the medical groups themselves scored higher under the Healthcare Effectiveness Data and Information Set, or HEDIS, a measurement tool developed by the National Committee for Quality Assurance.
Humana also said it plans to make virtual care, or telemedicine, a benefit for all of its Medicare Advantage members in 2020, building on a pilot it first launched in 2018. Humana members in the pilot generally reported positive experiences with telemedicine, according to the report.






