In an attempt to lower insulin costs for members who receive prescription drug coverage through Medicare Part D or Medicare Advantage, several plans will limit out-of-pocket costs to a $35 copay. The Centers for Medicare and Medicaid Services (CMS) said this change would make insulin costs more consistent for patients and potentially reduce out-of-pocket costs by hundreds of dollars.
More than 1,750 Medicare Part D and Medicare Advantage plans will include this change in their plans for 2021.
Most Medicare patients choose to enroll in Part D coverage, either through a standalone prescription drug plan or through a Medicare Advantage plan. Roughly 75% of Medicare enrollees had Part D coverage last year, according to CMS.
Medicare Part D plans are divided into four phases. The amount that patients pay toward their prescription fluctuates with each phase.
For example, a patient would pay toward their deductible in the first phase, and would then be responsible for paying 25% of the drug cost before reaching an initial coverage limit, currently set at $4,020. After reaching that threshold, they go into the “coverage gap,” where the patient pays for 25% of the drug price and manufacturers cover most of the cost, before reaching their out-of-pocket limit. CMS estimated the average out-of-pocket cost for insulin each year would be $675 using this structure.
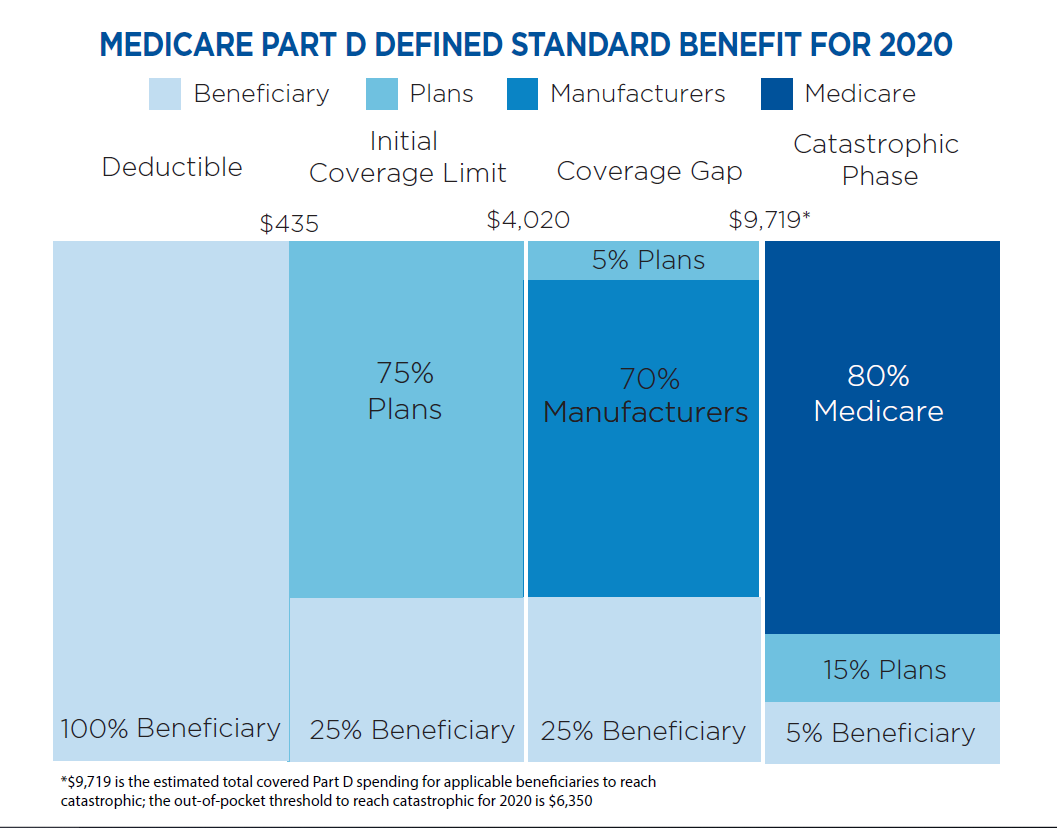
A chart shows how much patients currently pay for prescriptions during the four phases of Medicare Part D plans. Courtesy of the Centers for Medicare and Medicaid Services.

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
Under the new plan, patients would only pay a $35 copay through each phase, for an estimated out-of-pocket cost of $229.
“This market-based solution, in which insulin manufacturers and Part D sponsors compete to provide lower costs and higher quality for patients, will allow seniors to choose a Part D plan that covers their insulin at an average 66 percent lower out-of-pocket cost throughout the year,” CMS Administrator Seema Verma said in a news release.
As before, pharmaceutical manufacturers will still pay for 70% of insulin costs while patients are in the “coverage gap.” But those payments would be calculated before the application of supplemental benefits.
All three major insulin manufacturers — Eli Lilly, Novo Nordisk and Sanofi-Aventis — will participate in the program.
Photo credit: Hero Images, Getty Images

