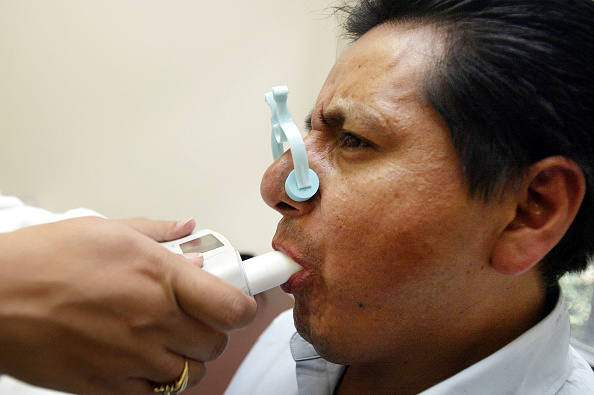
Vicente Benavidez blows into a spirometer to check for airway abnormalities at the World Trade Center Worker and Volunteer Medical Screening Program October 1, 2003 in New York City. Benavidez worked for four months removing asbestos from Ground Zero following the September 11, 2001 terrorist attacks. Photo credit: Mario Tama, Getty Images
The Food and Drug Administration issued a recent warning about the accuracy of pulse oximeters after a study found they missed low blood oxygen levels in Black patients more frequently than in white patients. But they’re not the only device that might have built-in racial disparities.
Researchers are also taking a closer look at spirometers — a device that is commonly used to help diagnose breathing conditions, such as asthma or chronic obstructive pulmonary disease. The devices are programmed with an automatic “correction” for lung capacity based on a patient’s race, adjusting for as much as a 15% lower lung capacity for Black patients, and as much as 6% lower for Asian patients.

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
But a growing number of researchers are warning that those assumptions, which have little scientific evidence, could further exacerbate racial disparities in patients’ outcomes from Covid-19.
In a commentary published in the Lancet in December, a group of researchers at UC San Diego warned that these adjustments could potentially cause clinicians to miss important diagnoses or influence treatment plans.
Although a spirometer would not be used while someone is contagious with Covid-19, it might be used to follow their recovery, including estimating the severity of any resulting lung damage.
“This will really matter for recovery from Covid,” said Amy Non, a genetic anthropologist at UCSD, who authored the Lancet paper. “It could influence estimates of severity of damage to the lungs after Covid. They could be underestimating the severity of the damage for Black patients.”
It could also influence factors such as whether patients are referred for pulmonary rehabilitation, or who can enter clinical trials for a drug that is being tested as a Covid-19 treatment. It’s difficult to know how much this is affecting patients’ recovery as the pandemic is still ongoing.
“What surprises me is that most clinicians I talk to have no idea that there is a racial adjustment built into this tool,” she said. “Our first mission is to raise awareness that there is a race adjustment and the research backing it isn’t strong.”
Her next goal is to document the clinical consequences of this adjustment, to see how patients would fare if it was simply removed from the equation.
Her work builds on years of research by Lundy Braun, a professor of medical science and Africana studies at Brown University, who wrote a book on the history of spirometers dating back to plantations.
She first learned about the race “correction” while reading an asbestos lawsuit, where it would be applied before determining what workers would be eligible for compensation.
According to her article, published in the Canadian Journal of Respiratory Therapy, the idea behind this “correction” dates back to slavery. Samuel Cartwright, a physician and slaveholder, might have been the first person to test differences in lung capacity based on race. And in the 1920s, in the midst of a eugenics movement in the U.S., the idea became further solidified in clinicians’ handbooks.
It still lingers in research today. After reviewing 226 papers that formed the basis for this “correction,” Braun found that less than one in five clearly defined race, and the vast majority did not include any measure of social class or geographic context.
“This is not just spirometry,” UCSD’s Non added. “There are so many historical biases that date back to slavery times that are still used in medicine today. It’s shocking.”








