No issue in healthcare or life sciences can be solved by a single stakeholder. As an example, effective chronic condition management needs a multidisciplinary care team and benefits from payment policies that reward value over volume. A similar principle applies to solving critical health equity issues. The complexity of social determinants of health demands partnership across the continuum of care, especially from entities outside the traditional care setting, and is vital to ensuring success.
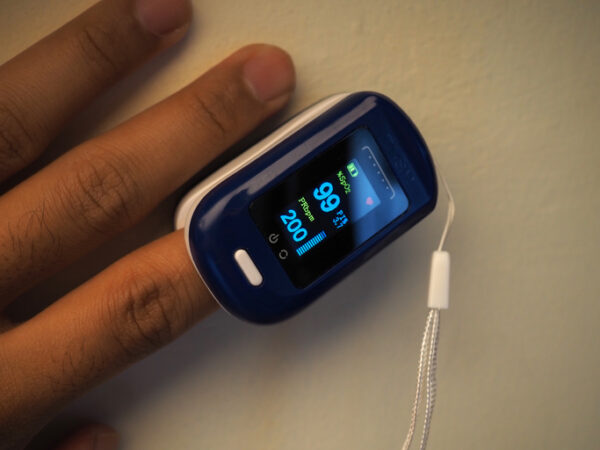
One recent example of this is pulse oximetry. This technology estimates the amount of oxygen in the blood using light and is used in emergency departments and intensive care units and many other care areas around the world to monitor patients with heart or lung problems and provides patient safety for all on general medical surgical wards and in the operating room. Indeed, since its inception some 30 years ago pulse oximetry is now considered the fifth vital sign and is virtually ubiquitous. Most recently, it has played a critical role in Covid-19 treatment by detecting decreases in blood oxygen saturation that aren’t accompanied by readily visible shortness of breath.
Unfortunately, pulse oximetry readings require light absorbance, which means readings aren’t always accurate for everyone as skin pigmentation absorbs light. In late 2020, a letter to the New England Journal of Medicine (NEJM) from five physicians at the University of Michigan Medical School pointed to an analysis showing that Black patients being monitored by pulse oximetry were nearly three times more likely to experience hypoxemia, or low levels of oxygen in the blood, than White patients.
That letter, and three subsequent studies published in 2022, showed that pulse oximeters don’t always provide accurate readings in patients with darker skin pigmentation. As a result, patients may not get the care they need right away, as clinical teams may not realize their blood oxygen is dropping. These studies are a start to understanding the complexity of the interface of devices and equity, but solving the performance gap requires a deeper understanding of the impact of skin pigmentation in addition to other factors, such as less than robust pulse signal quality caused by poor perfusion, and controlled study designs to confirm that changes are effective.
While some medical research gets put on a shelf and is rarely revisited, that hasn’t been the case here. Over the past two and a half years, a multidisciplinary effort has begun to confront the issue in an open and collaborative way – and the fast response should serve as a model for other important issues of equity that the industry must address.
Multidisciplinary work from regulatory bodies, non-governmental organizations, healthcare professionals and industry
In February 2021, the U.S. Food and Drug Administration (FDA) issued new guidance on taking and interpreting pulse oximeter readings for patients and healthcare providers. The agency said its communication was a direct response to the NEJM letter: “[T]he FDA agrees that these findings highlight a need to further evaluate and understand the association between skin pigmentation and oximeter accuracy.”

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
That wasn’t all, though. Last year, the FDA’s Medical Devices Advisory Committee reconvened its Anesthesiology and Respiratory Therapy Devices Panel, which was initially formed in 1995 and last met in 2018. The panel, comprised of representatives from academia, healthcare, regulatory agencies, non-governmental organizations like the International Organization for Standardization (ISO) and industry, used its November 2022 meeting to specifically address the accuracy of pulse oximeters in patients with darker skin pigmentation. For 2024, FDA has stated that draft guidance on clinical and scientific evidence for pulse oximeters is a key priority.
After reviewing comment submissions, presentations, and real-world evidence studies, the panel made several key recommendations for the industry. These include updating existing guidance on evaluating the full spectrum of skin pigmentation in clinical studies, updating labels on both prescription and over-the-counter pulse oximeters, and exploring additional assessments of pulse oximeter performance to help clinicians understand factors impacting device accuracy.
At the same time, a project founded at the University of California San Francisco called Open Oximetry is similarly convening stakeholders from multiple market segments to investigate the issue. The group has set a series of short- and long-term goals centered on testing and improving existing devices, developing models to predict pulse oximeter performance, develop more affordable, accurate devices, write new standards to account for factors impacting performance, and create open data repositories for use in product development. Critically, Open Oximetry is looking to answer an important and persistent question: Why do some pulse oximeters perform more accurately in the lab than in the clinical setting? In fact, they have undertaken a study, commissioned by FDA, to assess real-world pulse oximetry data that may help refine testing requirements for manufacturers.
Finally, there have been significant efforts in terms of how we evaluate social determinants of health — specifically, how skin tone stratification or colorism come into play. The implementation of the Monk Skin Tone Scale, which was developed to capture the complete spectrum of diversity of skin tone, allows researchers and clinicians to better understand how variations in skin tone can influence the accuracy of pulse oximetry readings. By utilizing this scale, the medical community can start to pinpoint discrepancies and work towards more equitable and accurate monitoring devices.
Industry partners need to play a role in collaboration
The work of the Anesthesiology and Respiratory Therapy Devices Panel and Open Oximetry shows the value of collaboration in addressing a pressing issue. By convening stakeholders who normally operate in silos, these groups can clearly define the problem and create a framework for developing the most effective solutions – and do so faster than any entity operating on its own.
When these conversations happen, it’s important to recognize the role that industry partners can play. Their expertise in patient/product education, product development, clinical trials, and post-market studies offers valuable perspectives to those less familiar with those processes. The relationships they’ve built can help connect investigators with similar interests who are working in different settings or geographies. They can commit their resources to proactively putting proposed guidelines into practice with products on the market or under development, as well as making efforts to educate clinicians on proper use of the technology. They also have the infrastructure to ensure clinicians are making proper use of their technologies in order to get the most accurate readings possible.
The large-scale, multidisciplinary effort to improve the performance of pulse oximeters shows the industry’s ongoing commitment to address inequities in care delivery. The effort also provides an example of the value of collaboration to solve problems that no single stakeholder can take on alone and shows how industry partners can contribute in a significant way when they have a seat at the table.
While there is still more work to do to improve guidelines and standards for use of pulse oximeters, we strongly believe that being united in purpose, our collective efforts can drive transformative change, ensuring equitable care for all.
Photo credit: Indra Pumama, Getty Images
Author Samuel Ajizian, M.D., FAAP, FCCM, CPPS is a board-certified Pediatric Intensivist with more than 20 years of clinical practice in the Pediatric ICU. He received his medical degree from the University of Southern California and completed pediatric residency and Chief Residency at Children’s Hospital Los Angeles. Dr. Ajizian joined Medtronic in 2015 in his first role as Vice President, Medical Affairs for the Patient Monitoring and Recovery business unit. In 2018, he assumed direction of the MITG Medical Safety Office. Dr. Ajizian then became interim director of the MITG Scientific Communications team, where he oversaw the production of key compliance-related deliverables including Clinical Evaluation Reports. In 2020, Dr. Ajizian assumed the roles of Chief Medical Officer of Patient Monitoring and Vice President of Global Clinical Research and Medical Science: Acute Care and Monitoring (formerly known as Patient Monitoring and Respiratory Innovations) at Medtronic.
Ashish K.Khanna, MD, FCCP, FCCM, is a staff intensivist & anesthesiologist, associate professor of anesthesiology and vice-chair for research with the department of anesthesiology, section on critical care medicine at the Wake Forest University School of Medicine, Winston-Salem, NC. He is a member of the Wake Center for Biomedical Informatics, the Center for Healthcare Innovation, the Wake Forest Hypertension and Vascular Research Cardiovascular Sciences Center and the Critical Illness, Injury and Recovery Research Center (CIIRRC). Dr.Khanna is a past chair of the Society of Critical Care Medicine’s (SCCM) In-Training Section and the SCCM Postgraduate and Fellowship Education Committee. He has more than 100 peer reviewed papers, and in addition two dozen book chapters, editorials, invited non-peer reviewed articles, and online educational videos to his credit and has been invited to talk about his work at prestigious national and international forums.
This post appears through the MedCity Influencers program. Anyone can publish their perspective on business and innovation in healthcare on MedCity News through MedCity Influencers. Click here to find out how.


