
One of the more famous precepts of Dr. William Osler (1849-1918), widely regarded as the Father of Modern Medicine and the “greatest diagnostician ever to wield a stethoscope,” was to, “treat the whole patient not just the disease.” The phrase he specifically used was, “the good physician treats the disease; the great physician treats the patient who has the disease.” He also insisted that “it is much more important to know what sort of a patient has a disease than what sort of a disease a patient has,” which recycles the axiomatic statement from Hippocrates that “it’s far more important to know what person the disease has than what disease the person has.” These are all words to live by for most physicians, even today.
The wisdom of these axioms notwithstanding, the editors of the scientific journal Oncologist channeled the zeitgeist and struck a chord with the scientific community when they reprinted an article from the Wall Street Journal entitled, “New era of personalized medicine: targeting drugs for each unique genetic profile.” The premise of this 1999 article, which debuted the memorable moniker, “personalized medicine,” runs directly counter to what Osler (and Hippocrates) preached, which was to care for individual patients rather than for their individual diseases, as explained below.
For context, a few months prior to the publication of this article, the FDA in September 1998 approved a monoclonal antibody called Herceptin or trastuzumab to treat metastatic breast cancer patients whose tumors overexpress the HER2 protein. Herceptin became the poster child for a new gene-based treatment paradigm or model, which uses DNA, RNA, receptors, or enzymes to guide medical decision-making and to subset genetically similar patients. A diagnostic test (HercepTest; Dako, Glostrup, Denmark) that stains the tumor tissue for the presence of HER2 overexpression was approved simultaneously with Herceptin to identify the most likely responders to it.

The Hidden Administrative Tasks Draining Small Practices
Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.
The success of Herceptin and the HerceptTest ushered in a new era of what became popularly and scientifically known “personalized medicine.” A catchy if somewhat inaccurate label, personalized medicine is often misinterpreted by the popular press and sometimes even by scientists and clinicians to mean holistic treatment of the person with special attention paid to individual patients’ preferences and interests, which is not really the case at all. Even though other more representative labels are now in use including “molecular medicine,” “stratified medicine,” “biologically personalized medicine,” “pharmaco-genetic medicine,” “individualized medicine,” and “precision medicine,” “personalized medicine” is unquestionably the O.G. and still the one most bandied-about in the media and society.
The irony of personalized or precision medicine (PM) is that it aims, against the advice of Hippocrates and Osler, to treat the disease, not the patient, based on his or her genetic profile and on any genetic alterations that are identified. PM essentially relegates to a back seat other patient-specific factors such as age, gender, family history, social and occupational circumstances, psychology, experiences, preferences, and lifestyle.
Another irony is that its highly precise therapies are perhaps too precise and well designed. Under the intense selective pressure of these therapies, diseases are forced to ‘Houdini’ their way out of eradication through the evolution of resistance, which broadly predisposes to treatment failure and worse clinical outcomes. This would seem to make a strong case for the use of a combination of targeted therapies that together block several, rather than one or a few, genes, proteins, or pathways. In some instances, like with the anti-HIV triple cocktail, that is the answer to the ever-present problem of drug resistance, but it usually comes at the cost of increased and possibly intolerable side effects.
Moreover, these therapies often target normal tissues, as well as diseased ones, since the proteins they block are widely expressed throughout the body and contribute to normal cell function along with disease progression. As a result, common side effects with targeted therapies are rash, diarrhea, high blood pressure, skin depigmentation, and thyroid, kidney, and liver damage.
Perhaps unsurprisingly, something of a backlash has set in against personalized medicine after the inflated expectations that attached themselves to it early on failed to materialize. This rise and fall of expectations perfectly describe the Gartner hype cycle which models the oscillation of events for a new treatment or paradigm when the initial bubble of enthusiasm is punctured by the subsequent needle of reality. What follows from this is either a period of recovery or continued disillusionment, as shown in the figure below.
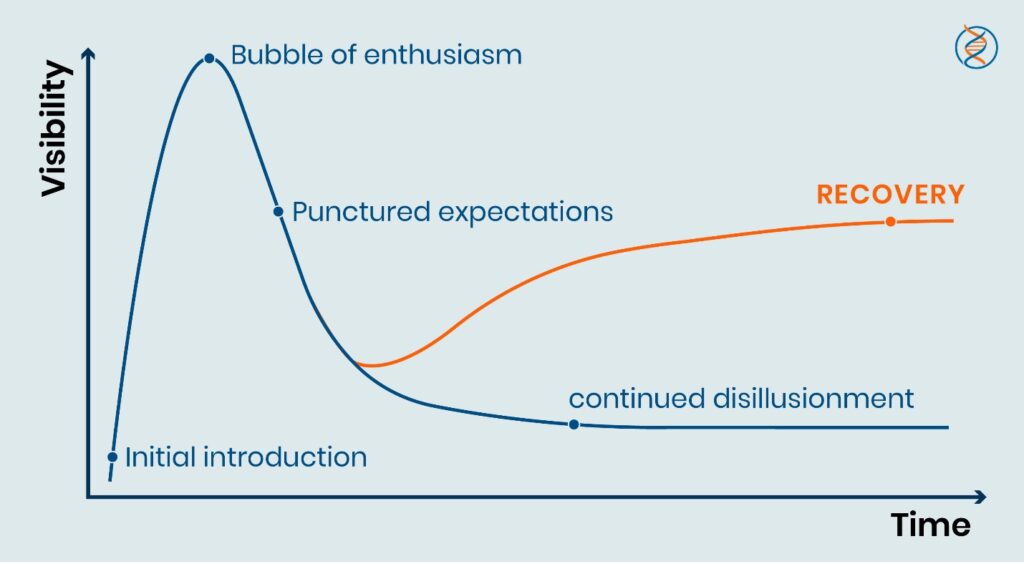
Image credit: EpicentRx
Possible next steps in the evolution of personalized medicine are therapies that target not specific genes, proteins or pathways per se but multiple abnormalities, which, because they are common almost exclusively to diseased tissues, spare normal ones from toxicity. The abnormalities that many diseased tissues share include overgrown and poorly constructed blood vessels, reduced oxygenation, low pH, excessive inflammation, and dysfunctional immune cell behavior.
This sounds a lot more like “personalized medicine” because it puts patients and their well-being first and foremost and the diseases which they suffer from second, even though both are, of course, inextricably linked.
Image: Getty Images, Yuuji
Dr. Bryan Oronsky serves as EpicentRx Chief Development Officer and combines firsthand clinical experience as a physician with 17 years of pharmaceutical development experience. EpicentRx’s pipeline includes treatments that are intended to not only reverse resistance to standard therapies like chemotherapy and checkpoint inhibitors but also to improve their tolerability. The company’s small molecule, RRx-001 is one of the most advanced direct NLRP3 inflammasome inhibitors in clinical development and has been evaluated in over 300 multimorbid cancer patients both alone and in combination with other therapies. RRx-001 has been evaluated in multiple independent studies for conditions where immune and inflammasome activation contribute to disease pathology. These include cancer, myocardial infarction, pulmonary hypertension, acute kidney injury, acute radiation syndrome (ARS), malaria, multiple sclerosis, Parkinson’s disease, and Alzheimer’s disease.
This post appears through the MedCity Influencers program. Anyone can publish their perspective on business and innovation in healthcare on MedCity News through MedCity Influencers. Click here to find out how.


