
Modern medicine is more advanced than ever, yet clinical care still leans heavily on what is, in practice, informed guesswork. Doctors make the most probable diagnosis, select the therapy most likely to help, and adjust only when outcomes fall short. To further complicate matters, one-half of patients with chronic diseases do not take their medications as prescribed.
Precision medicine offers a more dependable path forward. Instead of guesswork, a patient’s care is informed by an individual’s unique genomic and clinical profile rather than population averages. Add in the power of AI to interpret this complexity at scale, and personalized, evidence-driven treatment will be the emerging standard.
How does precision medicine work?

The Power Behind Enterprise EHR Software for Large Healthcare Systems
Enterprise EHR boosts scalability, interoperability, and governance for large healthcare systems.
Precision medicine tailors treatments and prevention strategies to the unique characteristics of each person. A simple analogy is a recruitment system that matches a candidate to a job based on specific education, experience, and skills to ensure the best possible fit.
To get started, precision medicine maps a person’s genomic profile using a sample of tissue, blood, or other body fluid. It’s looking at all the genes in a person or in a specific cell type and how they interact with each other and the environment.
This type of profiling helps explain why some people get certain diseases while others do not. It can also be performed on tumor tissue to look for mutations or other genetic changes that influence how different types of cancer form and respond to treatment. These insights can guide more accurate diagnosis, targeted therapies, and new prevention strategies. This work relies on genomic profiling platforms, EHR data, self-service analytics tools, visual and predictive modeling, machine learning, and other emerging technologies.
How can AI enable precision medicine and targeted patient treatment?
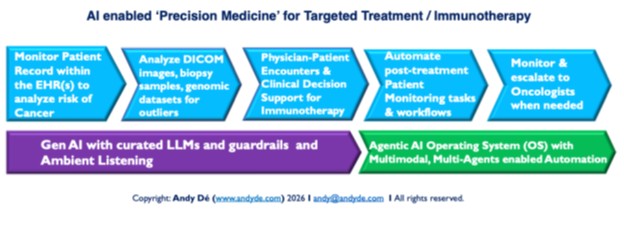
Figure 1. AI-enabled precision medicine for targeted treatment
Thanks to rapid advances in AI, spanning machine learning, deep learning, natural language models, and new agentic AI, precision medicine is moving from a research slogan to clinical reality. We’re now much closer to delivering targeted treatment for complex diseases like cancer, as shown in figure 1.
How does this differ? Traditional clinical guidelines tell us what works on average for a broad population. Precision medicine asks a more meaningful question:
“What is the right prevention, diagnosis, or treatment for this individual, right now, given everything we know about them?”
Generative AI (Gen AI) and agentic AI approach this challenge in complementary ways:
- Generative AI (LLMs) synthesizes large volumes of multimodal data, including text, images, genomic information, or molecular structures, into clear insights.
- Agentic AI goes a step further by reasoning, planning, and taking action across tools and workflows to help move a patient journey forward.
Together, they’re forming an intelligence and orchestration layer that brings truly personalized care within reach.
What Gen AI makes possible in precision medicine
- Predicting disease-risk years in advance
A new wave of generative AI models is pushing risk-prediction far beyond single-disease scores.
In 2025, European researchers released Delphi-2M, a generative AI model that predicts an individual’s risk of more than 1,000 diseases up to 20 years in advance. Trained on 400,000 UK Biobank patients and validated on 1.9 million people in Denmark, it uses LLM-style architectures applied to longitudinal health records to forecast complex clinical trajectories rather than just one outcome.
For precision medicine, tools like this can:
- Identify patients who may develop heart failure, diabetes, sepsis, or cancer long before traditional risk models detect a concern.
- Enable personalized prevention programs, screening schedules, and lifestyle recommendations tuned to each person’s projected disease pathway.
- Using genomics and biomarkers to guide targeted therapies
Gen AI models are becoming critical for turning genomic and molecular data into actionable, personalized treatments.
Recent reviews in Frontiers in Medicine and other journals highlight how ML and generative models are being used in precision oncology to identify new biomarkers, predict treatment response, and stratify patients for targeted therapies. At Memorial Sloan Kettering, researchers are building advanced ML and generative models to support precision cancer care in pediatrics.
For precision medicine, these capabilities make it possible to:
- Detect molecular markers that indicate which therapies a patient is most likely to respond to.
- Tailor treatment plans based on predicted response patterns rather than broad tumor type alone.
- Personalized treatment plans and care instructions
On the front lines of care delivery, Gen AI is already generating personalized decision-support insights.
Models can integrate a patient’s full medical history, genomic profile, comorbidities, and real-time wearable data to draft personalized treatment plans. For example, treatment plans could include optimal medication titration schedules for hypertension paired with behavior-change goals tailored to physical activity patterns and social determinants.
LLMs then translate these plans into patient-friendly education, adapted to literacy level, language, cultural context, and preferred medium (text, visual, or audio). In short, Gen AI is becoming the cognitive engine that turns raw, multimodal data into individualized care guidance.
Agentic AI as the operating system for personalized care
While Gen AI can generate insights, it’s not enough on its own. Healthcare needs a way to put those insights into action. That’s where agentic AI comes in. These systems can observe data, reason over guidelines and patient preferences, plan multi-step workflows, and act while keeping clinicians in the loop when needed.
Early systems like AgentClinic and autonomous clinical assistants show how these agents can support documentation, triage, diagnosis, and training. In essence, agentic AI provides the operational backbone that turns precision-medicine insights into consistent, coordinated action.
Use Case: Patient path from detection to treatment
To see how these technologies come together in practice, consider a simplified patient journey:
- Initial detection: During a routine checkup or blood test, a liquid-biopsy tool paired with AI (e.g., MIGHT) detects abnormal ctDNA fragments that may signal an early-stage tumor.
- Diagnostic confirmation: On suspicion, clinicians order genomic sequencing of the tumor (or more detailed molecular testing) to understand what is driving the tumor.
- Molecular insights: Using a precision oncology platform, the care team reviews the tumor’s biomarker profile to identify actionable mutations or vulnerabilities.
- Targeted therapy selection: Based on the molecular profile, the patient is offered a targeted therapy or immunotherapy, rather than a generic “one-size-fits-all” chemotherapy regimen.
- Post-treatment monitoring: After treatment, periodic liquid-biopsy tests track ctDNA levels (MRD). Shifts in these levels can flag early signs of relapse, allowing clinicians to intervene sooner.
Conclusion:
Gen AI and agentic AI are already shaping what precision medicine can deliver, helping clinicians detect disease earlier, choose more effective therapies, and monitor patients with far greater clarity. The larger opportunity lies in embedding this approach across the lifespan. What if genomic profiling became a routine part of early care and a standard element of every patient’s electronic record?
While there’s a lot to unpack in that question, particularly around privacy and ethical standards, take a moment to think about that future. Precision medicine offers a path for healthcare to become more proactive, more personalized, and more effective for every individual with a far more sustainable cost curve. Of course, in everything we do with AI, privacy and ethics need to be handled with the utmost care and thoughtfulness. And while it won’t be easy, the alternative is to continue a model that reacts late, treats broadly, and spends heavily.
In short, AI-enabled precision medicine offers a rare combination of better outcomes, better experiences, and better value. It brings us closer to a healthcare system that treats each individual as a cohort of one. The question now is how quickly we are willing to move toward that future.
Photo: ipopba, Getty Images
Andy Dé is the chief marketing officer (CMO) at Lightbeam Health Solutions, a leader in population health management (PHM) and value-based care (VBC) Enterprise SaaS solutions for healthcare providers, payers and employers. In this role, he leads the global marketing organization and is responsible for go-to-market (G2M) strategy, planning and execution.
This post appears through the MedCity Influencers program. Anyone can publish their perspective on business and innovation in healthcare on MedCity News through MedCity Influencers. Click here to find out how.


