
Highmark, Lark Health extend collaboration
The expanded partnership increases the number of Highmark health plan members eligible for enrollment in Lark Health's AI-driven health coaching programs aimed at managing and preventing chronic diseases.

The expanded partnership increases the number of Highmark health plan members eligible for enrollment in Lark Health's AI-driven health coaching programs aimed at managing and preventing chronic diseases.

A new survey of U.S. physicians shows that they have differing views on how the payer market needs to evolve, but a vast majority agree that affordable insurance is necessary to provide access to high-quality care while reducing costs.

Munck Wilson Mandala Partner Greg Howison shared his perspective on some of the legal ramifications around AI, IP, connected devices and the data they generate, in response to emailed questions.

The final rule requires insurers to disclose information on prices for healthcare services and cost-sharing with patients. The government says it will help lower prices, but insurers aren't so sure.
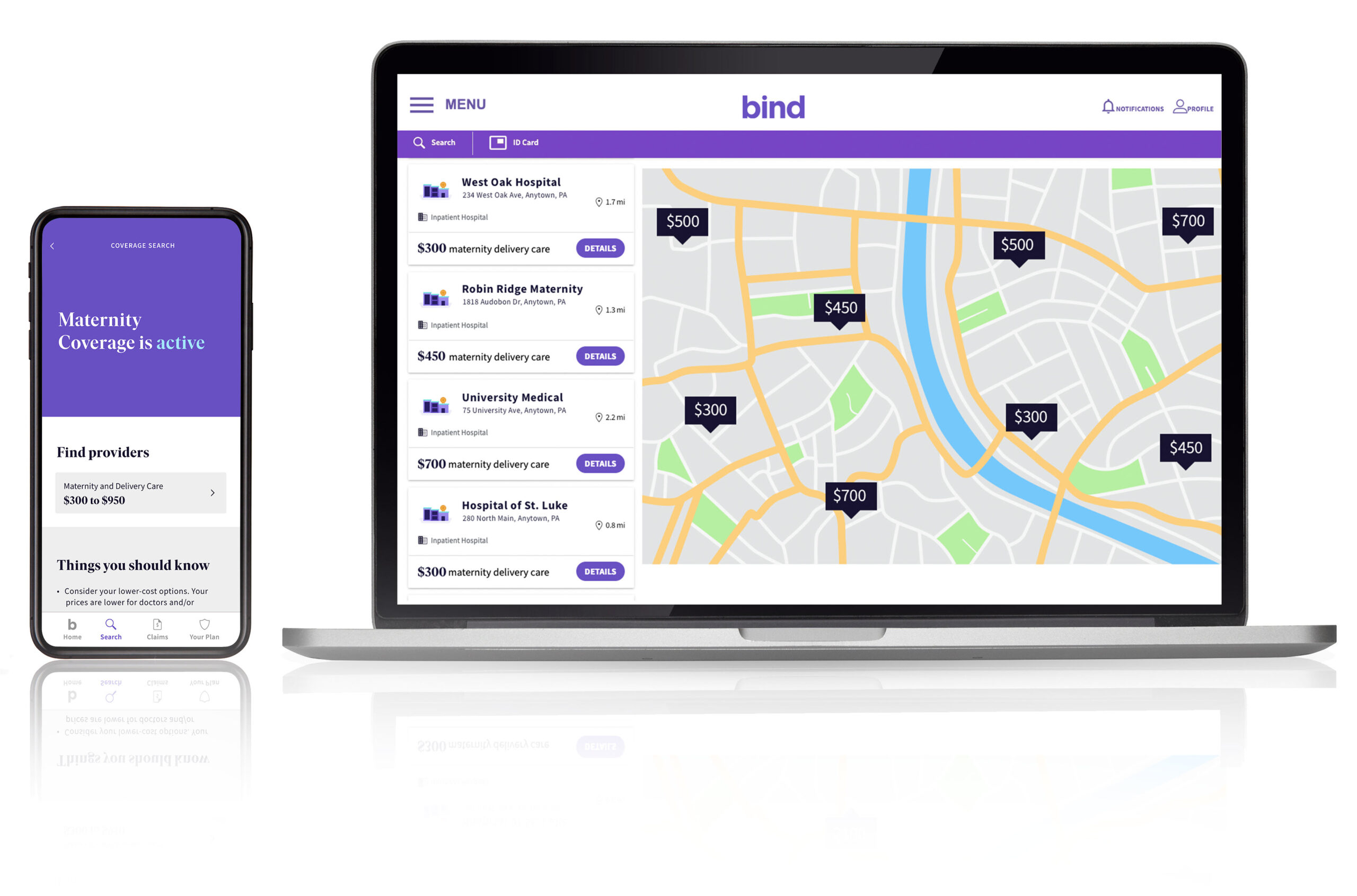
Insurance startup Bind Benefits just raised $105 million in a Series B funding round to further expand into the fully insured market. CEO Tony Miller sees the company's health plan product as a way for employers to stay agile while offering insurance in a rapidly changing world.

The insurance giant will expand its existing partnership with telehealth provider MDLive.

Through their partnership, the companies will integrate DocASAP's real-time online scheduling with HealthSparq's provider and cost search capabilities in one platform.

A new survey of 120 payers found that while health insurers see the positive impact of value-based care initiatives, challenges still remain, particularly regarding innovation and analytics.

Earlier this week, Aetna sued claims administrator Kurtzman Carson Consultants, the company that was tasked with sending settlement notices to up to 12,000 Aetna members last year. Shortly thereafter, KCC fired back with a lawsuit against Aetna. The organizations blame each other for breaching Aetna members' privacy.

In a recent phone interview, Humana CMO Dr. Roy Beveridge chatted about value-based care, social determinants of health, 2018 predictions and what the Louisville, Kentucky-based payer has been up to.

In a recent phone interview, Roswell, Georgia-based Tea Leaves Health President Miki Kapoor chatted about his company being acquired by Welltok earlier this year. He also discussed his career, physician engagement and his predictions for healthcare in 2018.

Gabby Everett, the site director for BioLabs Pegasus Park, offered a tour of the space and shared some examples of why early-stage life science companies should choose North Texas.

The state said it identified 245 grievance-system violations during this latest investigation of consumer complaints at Anthem from 2013 to 2016.

Founded by executives from MD Revolution and Nucleus Health, San Diego-based MintHealth has launched a personal health record built using blockchain technology.

During the keynote at MedCity INVEST Twin Cities, Zipnosis cofounder and CEO Jon Pearce discussed how the three amigos of healthcare — the patient, the provider and the payer — are key to digital health adoption.

How do the big five health insurers — Aetna, Anthem, Cigna, Humana and UnitedHealthcare — utilize social media? And which ones do the general public view in the most positive light?